To many people, poor dental health translates to cavities and crooked teeth. However, it can encompass more than these well-known phenomena and include problems such as gingivitis and periodontitis. While these words may sound like an exotic foreign language, their effects — also called gum disease — are more common than you may think. Nearly half of people over 30 have some form of gum disease, and the percentage increases to 70 percent in people over 65.
What Is Gum Disease?
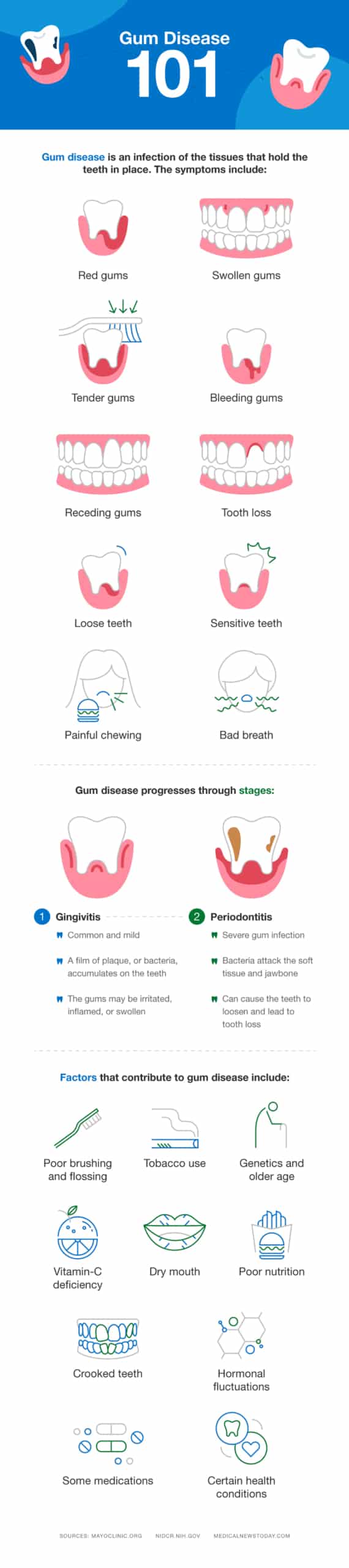
Also known as periodontal disease, gum disease occurs when the soft tissue that keeps the teeth in their proper positions becomes infected. Without timely treatment, the infection can damage the jawbone causing the teeth to loosen or fall out. Research also suggests gum disease may impact other areas of the body: Researchers have linked it to diabetes, heart disease, rheumatoid arthritis, and other conditions.
What Are the Stages of Gum Disease?
Gum disease may begin innocently, but over time it can cause serious problems. Gum disease has two stages.
Gingivitis
Gum disease starts as gingivitis. What is gingivitis? The word may sound unusual, but like many words it takes its roots from the Latin gingivae, referring to the gums, and the suffix -itis indicating inflammation. As the word suggests, this condition primarily consists of gum inflammation. It’s the earliest and mildest stage of gum disease, and it’s quite common.
Periodontitis
Left untreated, gingivitis can progress to periodontitis. What is periodontitis? This condition is the second stage of gum disease, and it happens when bacteria and infection attack the jawbone. It’s a serious infection of the gums that can also harm the soft tissue and cause the teeth to loosen. As it progresses to advanced periodontal disease, the bacteria does even more damage to the bone and can cause pus-oozing gums, severe bad breath, and more loosening of the teeth.
What Causes Gum Disease?
Many factors can contribute to gum disease. Most often, gingivitis results from poor brushing and flossing habits. When the sugars and starches in food encounter normal mouth bacteria, they form a sticky film known as plaque. If a person doesn’t remove plaque thoroughly and regularly, it hardens into tartar or calculus under the gumline which makes the plaque harder to remove. In this situation, bacteria can thrive which irritates the gums around the base of the teeth and leads to inflammation, swelling, bleeding, and other symptoms of periodontal disease.
While poor oral hygiene is the most common cause of gum disease, many other factors can play a role. Genetics and older age can increase one’s odds of issues as can unhealthy habits such as smoking, chewing tobacco, and poor nutrition, including a vitamin-C deficiency. Other oral conditions such as having a dry mouth, crooked teeth that are difficult to brush and floss, and ill-fitting dental restorations can also lead to sub-optimal dental and gum health.
In addition, hormonal fluctuations from pregnancy, the menstrual cycle, or birth control pills can impact gum health, as can certain medical conditions, including some infections. People who are immunocompromised due to a health problem such as HIV/AIDS or cancer treatment may have an increased risk of gingivitis and gum issues. Taking certain medications such as some for angina, high blood pressure, and epileptic seizures may also increase the risk.
How Do You Know if You Have Gum Disease?
Knowing you have gum disease is key but it’s not always self-evident. Gingivitis is frequently painless and therefore easy to overlook. Watch for these signs to catch this problem early while the damage may still be reversible. In a healthy mouth, the gums are pale pink, firm, and snug around the teeth. In people with gingivitis, the gums lose this healthy appearance and instead can be swollen, puffy, and dark red. They may recede and bleed when flossing or brushing. People with gingivitis may have bad breath.
While some of the symptoms of periodontitis overlap with gingivitis, they tend to be more intense. You may see more redness and swelling and notice enough bleeding to cause your toothbrush to turn pink. You may even spit out blood when flossing or brushing. Your gums may feel tender to the touch and chewing may cause discomfort.
As periodontitis worsens, new spaces may form between the teeth, and pus can collect between the teeth and gums. The teeth may even move to the point that they don’t fit together in the same way when biting. If the situation grows serious enough, your dentist may need to remove the affected teeth.
How to Prevent Gum Disease
The good news is gum disease is largely preventable with the right amount of strategy and effort. Practicing proper oral hygiene is key. Brush your teeth for two minutes at least twice a day in the morning and at night. Floss your teeth at least once a day before brushing to loosen food particles and bacteria, so you can then brush them away. For even better results, brush your teeth following each meal or snack throughout the day.
Visit the dentist regularly for check-ups and cleanings. Typically, dentists recommend a cleaning every six months to once a year, but people who are more susceptible to periodontitis may need to go more frequently. Annual X-rays can reveal gum issues not visible during an examination. A dental visit is also a great time to perfect flossing and brushing techniques. Show the hygienist how you clean your teeth at home and see if they have tips to get your teeth cleaner, brighter, and whiter.
How to Treat Gum Disease
Treating active gum disease is critical to one’s mouth and overall health. Fortunately, you can opt for a variety of treatments depending on the stage and situation. Your dentist or hygienist may recommend the following therapies.
Scaling and root planing
Dental professionals perform these non-surgical procedures by applying a local anesthetic. First, they scale the teeth by scraping away the plaque and tartar above and below the gum line. Then they may plane the roots by smoothing rough spots to remove bacteria and create an optimal surface for the gums to reconnect to the teeth.
Antibiotics
Your dentist or periodontist may prescribe these medicines to decrease or eliminate the bacteria involved in gum disease. They may use them alone or as part of a treatment regimen involving surgery or another therapy.
Flap or pocket reduction surgery
During this procedure, a periodontist flaps the gums back to remove tartar and then replaces the tissue tightly around the tooth to decrease the space where bacteria can thrive.
Grafts
In spots where the gums are thin or have receded, a periodontist can graft tissue, typically from the roof of the mouth, and add it to the trouble area. For people who have suffered bone destruction, a bone graft can provide a base for bone to regrow to help stabilize the teeth.
Guided tissue regeneration
A periodontist may do this procedure along with flap surgery. They’ll add mesh-like fabric to an area between the gum tissue and bone to allow the bone and connective tissue to thrive without having to compete with gum tissue growing in the way.
Tissue-stimulating proteins
A periodontist may apply a special gel, which consists of proteins from developing tooth enamel, to the diseased tooth root to encourage the growth of bone and tissue.

How to Improve Gum Health at Home
The best approach to gum disease is to prevent it before it starts or escalates. Consider these at-home measures.
Switch to an electric toothbrush
Consider using an electric toothbrush when brushing, which may be more effective than a manual toothbrush. Otherwise, opt for a toothbrush with soft bristles, and replace it every three months or sooner.
Use an interdental cleaner
In addition to brushing and flossing, clean between your teeth with an interdental brush, dental pick, or dental stick. Research suggests this practice can reduce plaque and improve gum health.
Use mouth rinse
Mouth rinse can combat bad breath. Used twice daily, it may also help keep gum disease at bay through its anti-gingivitis properties. While not a substitute for brushing and flossing, you may benefit from adding it to your regular dental hygiene routine to reach areas of the mouth and teeth that are hard to access with a toothbrush. Many varieties are available by prescription and over the counter.
Improve your overall health
Finally, you’ll encourage a healthy mouth when you transition to a healthier lifestyle. Research suggests that eating a diet low in carbohydrates and rich in Omega-3 fatty acids, vitamins C and D, antioxidants, and fiber for four weeks can cut gum inflammation in half. Quitting smoking can also go a long way toward improving your gum health, since tobacco use is a major risk factor for periodontitis.

Conclusion
When you think of healthy teeth, you may think of a bright smile full of pearly whites. But oral health is much more than that. The next time you’re tempted to skip brushing or flossing, envision removable plaque turning into stubborn tartar — and get cleaning.
Reviewed By
Dr. Elizabeth Clary, D.M.D. is a member of the American Dental Association, Missouri Dental Association, Missouri Academy of Pediatric Dentistry, Chicago Dental Society, Greater St. Louis Dental Society, and Southern Illinois University School of Dental Medicine Alumni Association.

