Good dental habits are crucial to keep your mouth — and body — in tip-top shape. Brushing and flossing regularly along with other proven steps can help prevent everything from cavities to gum disease, including the severe form of gum disease called periodontitis.
What is Periodontitis?
Gum disease develops in several stages, beginning with inflammation known as gingivitis. If left untreated, this milder form of gum disease can develop into periodontitis, a more significant dental issue that can lead to mouth infections and loose teeth.

The good news is proper oral hygiene can work wonders. Those who take good care of their teeth and gums can prevent gingivitis from developing in the first place. Others who suffer from gingivitis can stop it from turning into periodontitis by improving their dental care.
Causes of Periodontitis
While we may not want to think about it, our mouths contain about 700 different kinds of bacteria, fungi, and other microbes. Many of them are harmless and even helpful.

When the mouth’s normal bacteria encounter the sugars and starches found in food, the two interact and can create a colorless, sticky substance called plaque. If you don’t remove plaque within 72 hours, it can harden into tartar on the teeth and under the gums. Tartar is problematic for several reasons. The bacteria in it may be unhealthy for the teeth and mouth. Plus, you can’t get rid of tartar by brushing and flossing. A dental professional must remove it during a cleaning.
Plaque and tartar can initially cause gingivitis leading to irritated and inflamed gums. If you don’t properly treat gingivitis, periodontitis can develop and put the health of the teeth and body at risk.
Risk Factors for Periodontitis
Poor oral hygiene — including not regularly brushing and flossing — is the number one cause of periodontitis. However, other factors can make a person more susceptible.
Age
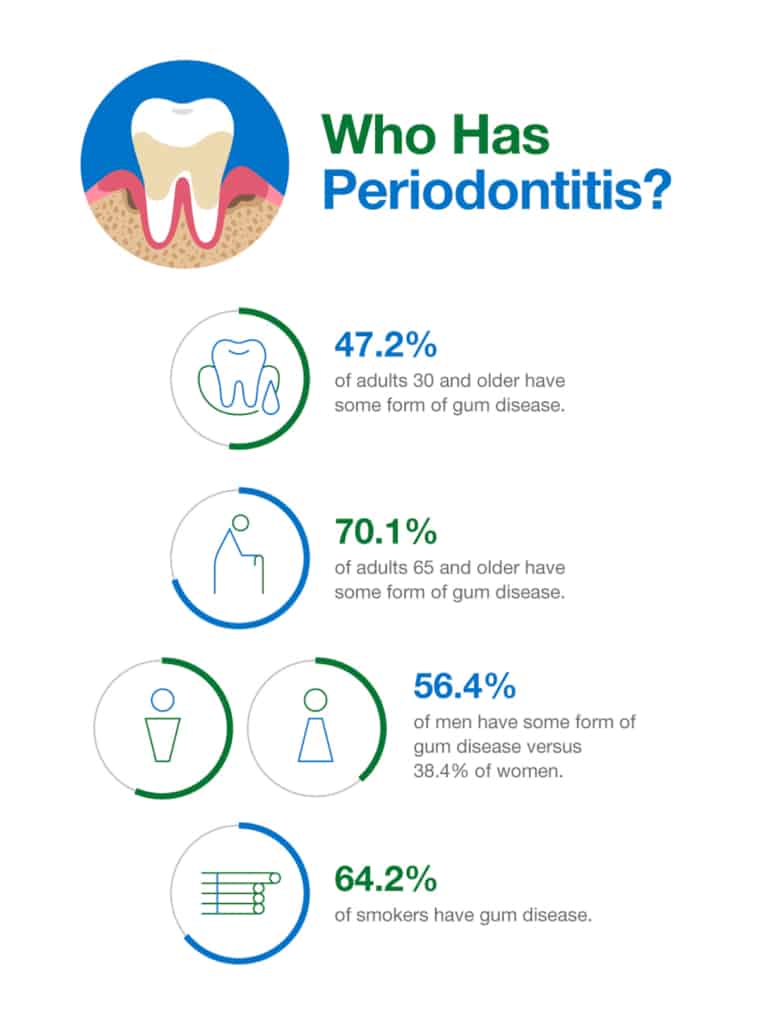
While gum disease is not unheard of in people younger than 30, close to half of all adults older than 30 have it in one form or another. By the time people are 65 and older, the number is seven in 10.
Gender
Gum disease tends to be more common in men with about 56 percent of males and 38 percent of females suffering from it. While women may be less likely to have gingivitis or periodontitis, their likelihood of experiencing it can increase during times of hormonal change such as during pregnancy or menopause.
Genetics
If you have one or more family members with gum disease, you’re more likely to develop it.
Lifestyle choices
Smoking increases your odds of developing gum disease. Nearly 65 percent of smokers have gingivitis or periodontitis. People who chew tobacco, vape, or use recreational drugs, such as marijuana, also have a greater likelihood of gum disease.
Health conditions
Obesity, diabetes, and rheumatoid arthritis can increase your risk of having gum disease. Not getting enough nutrition including vitamin C can make gum disease more likely. Illnesses that decrease immunity such as HIV, AIDS, and leukemia can also increase a person’s risk.
Dry mouth
Taking medications that decrease the production of saliva can increase your likelihood of getting gum disease. Some of these medications include antidepressants, antihistamines, and blood-pressure drugs.
Periodontitis Symptoms
Symptoms of gum disease can start mildly for people with gingivitis and become more serious for those with periodontitis. Warning signs include gums that are bright red or purplish and swollen or puffy instead of pink and firm. Gums that are tender to the touch and bleed easily also signal a problem. Bad breath can be a warning sign too.
As gingivitis progresses to periodontitis, symptoms can become more severe, and new, concerning ones can appear. For example, bleeding can worsen from observing pink-tinged toothbrush bristles to spitting out blood after flossing or brushing.
The best way to determine if you have periodontitis is to visit your dental health professional. The dentist can take a thorough medical history and ask about any health issues or lifestyle factors that may put you at higher risk for gum disease. In addition, your dental team will conduct a thorough visual examination, including checking if there is any inflammation of the gums and measuring any pockets around the teeth with a tiny ruler. They may also take X-rays to check for possible bone loss.
Advanced Periodontitis
If undiagnosed and untreated, gingivitis and then periodontitis can lead to advanced periodontitis. At this stage, more significant damage can occur. Pus may form between the gums and teeth, and problems with the teeth can develop if the gums recede. Teeth may become loose which can lead to other changes. For example, new spaces may form between them, your bite may shift, and chewing may become painful. If periodontitis becomes advanced, it can result in tooth loss.
It may also affect your overall health if bacteria get into the bloodstream from the gum tissue. Researchers have linked coronary artery disease, respiratory disease, and rheumatoid arthritis to periodontitis. In addition, advanced periodontitis can make it harder for people with diabetes to control their blood sugar.
As with periodontitis, your dentist can diagnose advanced periodontitis and recommend a treatment plan.
Treatments for Periodontitis
A number of treatments are available for periodontitis. Your dental team will determine the specific regimen based on the severity of gum disease. Typically, care begins with a thorough cleaning of the teeth and gums by a periodontist (gum specialist), dentist, or dental hygienist.
When your dental providers catch periodontitis early enough, they can do less invasive treatments. Often, they will use instruments, such as an ultrasonic device or a laser, to get rid of the tartar on the surfaces of the teeth and under the gums. They can also smooth the root surfaces to try to prevent any more buildup.
Your dentist or periodontist may prescribe antibiotics to treat an infection. They may also prescribe an antibiotic mouth rinse or gel to put between the teeth or into gum pockets as well as oral antibiotics to eliminate the bacteria causing the infection.
If periodontitis has advanced, one or more of these surgeries may be necessary.
Flap surgery
Also known as pocket reduction surgery, this procedure involves peeling back a section of the gums for better access to the roots that need scaling and root planing. If bone loss has occurred, the surgeon may recontour the bone as well.
Bone graft
If the bone is destroyed around the root of the tooth, a bone graft may be necessary to keep the tooth in place to hopefully prevent its loss. The dentist can make the graft from your bone, donated bone, or synthetic bone, and the graft may provide a platform for the natural bone to regrow.
Guided tissue regeneration
In this procedure, the dentist or periodontist places a specialized biocompatible fabric between the tooth and bone to block unwanted tissue from getting into the area and to encourage the bone to grow back.
Tissue-stimulating proteins
Finally, the dentist or periodontist can encourage the bone and tissue to grow back by applying a gel to the affected tooth root. The gel consists of proteins found in developing tooth enamel.
Ways to Prevent Periodontitis
The best way to prevent periodontitis is to stop it from occurring in the first place. Practicing good oral hygiene is the single most effective method.
Brush morning and night at a minimum — or better, after every meal. And don’t forget your tongue. Use a soft-bristled toothbrush and replace it every three to four months. An electric toothbrush typically removes plaque better than brushing by hand. Select a toothpaste that has the approval of the American Dental Association (ADA) and contains fluoride.
Floss at least once a day to remove plaque and food that the toothbrush can’t reach. In addition, use a dental pick, dental stick, or interdental brush for greater access to hard-to-reach areas. Similarly, an alcohol-free mouth rinse with anti-gingivitis properties can play a role in keeping the mouth healthy.
Practicing positive lifestyle habits is also important. Get regular dental cleanings to catch problems before they become serious. Quit smoking and chewing tobacco if applicable and eat a well-balanced nutritious diet.
Conclusion
Periodontitis with its threat of potential tooth loss can be scary. Fortunately, a combination of good oral hygiene and regular dental care can help keep your gums healthy and provide enough notice for your dentist to help you detect and reverse any potential issues.
Reviewed By
Dr. Elizabeth Clary, D.M.D. is a member of the American Dental Association, Missouri Dental Association, Missouri Academy of Pediatric Dentistry, Chicago Dental Society, Greater St. Louis Dental Society, and Southern Illinois University School of Dental Medicine Alumni Association.


